| Table of Contents |  |
|
Case Report
| ||||||
| A rare giant gynecomastia and an abnormal 46XY 15ps+ karyotype in a 15-year-old boy | ||||||
| Manuneethimaran Thiyagarajan1, Pragnya Chigurupati2, Balaji Singh K.3 | ||||||
|
1MS, Assistant Professor, General Surgery, Sri Ramachandra Medical University Porur, Chennai, India.
2MBBS, Postgraduate, General Surgery, Sri Ramachandra Medical University Porur, Chennai, India. 3Professor and Head of Department, General Surgery, Sri Ramachandra Medical University Porur, Chennai, India. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article: |
| Manuneethimaran T, Chigurupati P, Singh BK. A rare giant gynecomastia and an abnormal 46XY 15ps+ karyotype in a 15-year-old boy. Edorium J Surg 2014;3:10–13. |
|
Abstract
|
|
Introduction:
Gynecomastia is one of the common endocrine disorders in adolescent boys. During puberty, up to 70% of the boys have some breast development. However, in this enlargement, up to 75% of the cases resolve spontaneously within 2 years without any treatment. Rarely surgical management is also required to correct the gynecomastia.
Case Report: A 16-year-old boy presented to us with gynecomastia, with a chromosomal aberration of 15ps+. We proceeded with a subcutaneous mastectomy using an infra areolar incision. Conclusion: The 46XY karyotype with enlarger satellites of acrocentric chromosome 15ps+, is one of the rare entities. Occurrence of Giant gynecomastia in the presence of this particular chromosomal aberration is also a rare entity. In this paper, we would like to highlight these rare entities and the management of the same. | |
|
Keywords:
Abnormal karyotype with gynecomastia, Giant gynecomastia, Gynecomastia, Subcutaneous Mastectomy
| |
|
Introduction
| ||||||
|
Benign enlargement of breast tissue in male is called gynecomastia. Most commonly adolescent boys are affected by this disorder. During the period of puberty up to 70% of boys have some breast enlargement [1]. However, in this enlargement up to 75% of cases resolve spontaneously within two years without any treatment [2]. Endocrine variation in boys with altered ratio of estrogen and progesterone is the reason for development of gynecomastia. One of the most common syndrome associated this kind of endocrine disorder is Klinefelter syndrome in which patient will have hypogonadism and gynecomastia with karyotype 46XXY. | ||||||
|
Case Report
| ||||||
|
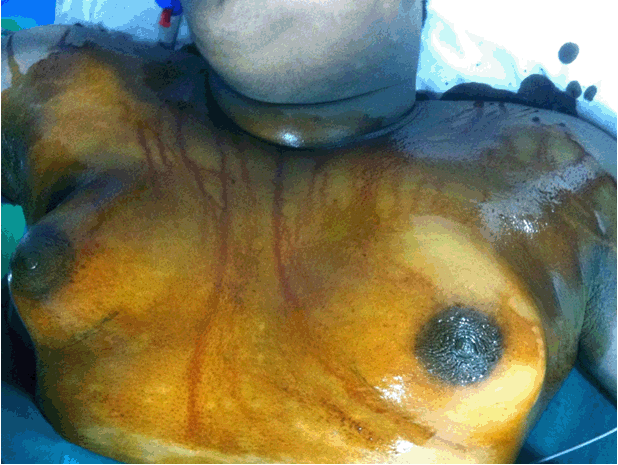
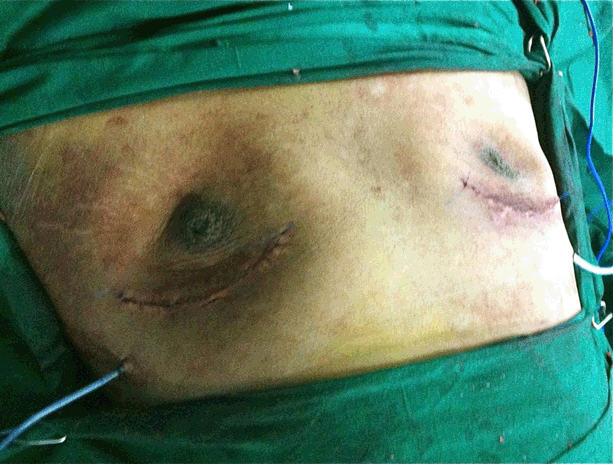
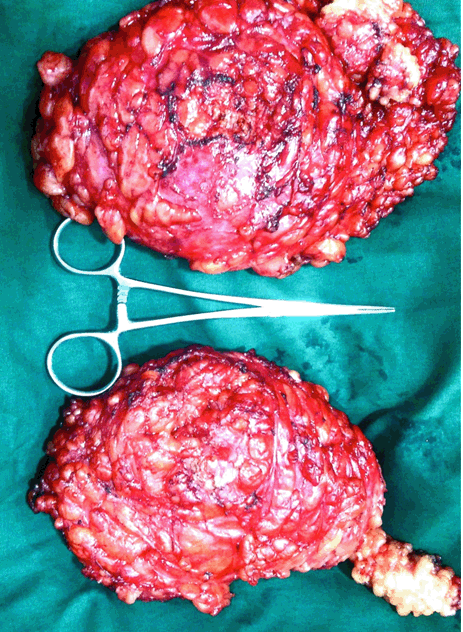
A 15-year-old boy came to our hospital with huge bilateral breast enlargement and with psychological depression. Clinical examination showed bilateral gigantic breast with size of 15x15x10 cm. But his external genitalia testis and penis size were normal. Complete evaluation was done to rule out the causes of gynecomastia. Biochemical analysis of the patient showed: In this biochemical analysis, hormone levels are nearly normal for tanner stage 1 and 2. Molecular analysis in peripheral leucocyte was done which showed normal male karyotype 46XY with chromosomal aberration in 15ps+. Ultrasonogram of abdomen was done to rule out female gonads in pelvis but it was normal. Computed tomography scan of brain was normal. The patient was advised against hormonal therapy by the endocrinologist. He was planned for a subcutaneous mastectomy. Using an infra areolar incision on both the breasts, complete breast tissue was removed. Postoperative period was uneventful and the patient was relieved of his undue stress. | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
The word gynecomastia is derived from Greek. Gyne means women and masto means breast. Gynecomasty is a synonym, and gynecomazia is an obsolete term. The most applicable definition of gynecomastia is "a benign enlargement of the male breast" (mamma masculina) [3]. The imbalance between estrogen action relative to androgen action at the breast tissue level appears to be the main etiology of gynecomastia [4]. The balance between free testosterone and estrogen is also affected by serum levels of sex hormone-binding globulin, which is the proposed mechanism of gynecomastia in certain conditions, such as hyperthyroidism, chronic liver disease, and the use of some medications such as spironolactone [4]. The endocrine imbalance can be divided into three categories [5]:
However, most cases are idiopathic [5]. It is divided into two categories:
Etiology wise, in primary hypogonadism, there is decreased synthesis of testosterone and increased peripheral conversion to estradiol, which leads to gynecomastia. In Klinefelter syndrome, which is associated with hypogonadism and gynecomastia, there is an increased risk of cancer–10–20% higher than in women [6]. In our patient, karyotype is 46XY with chromosomal aberration in 15ps+. In this particular karyotype we can notice enlarged satellites of acrocentric chromosome (15 ps+). Chromosomal aberration can occur in both sex chromosome and autosomal chromosomes. It can be a numerical abnormality or structural abnormality. The structural abnormality in autosomal chromosomes is 15pst. Chromosomal disorders account for 11.3% in population suspected to have genetic disease and the chromosome abnormalities amount to 7.5%. Most of the chromosomal abnormal fetuses are eliminate by miscarriages, still the frequency of abnormalities in live borns is about 0.6% [7]. Patients with 15ps+ karyotypes can be associated fetal anomaly, hypospermatogenesis and infertility [8] [9] only cases with numerical abnormality in sex chromosomes are associated with gynecomastia. In review of literature, casual relationship or co-occurrence of gynecomastia in the presence of 15ps+ karyotype was not so far reported. In our case, gynecomastia was very huge. Although there is no definitive evidence for casual relationship between gynecomastia in the presence of 15ps+ karyotype, we can consider this as a first time co-occurrence. According to Webster's classification gynecomastia can be divided into three types: Glandular type, Fatty glandular type and simple fatty type. Glandular type is treated by surgical removal of the gland, fatty glandular type requires surgical removal along with liposuction and simple fatty type will benefit from liposuction [10]. Since our patient had more of glandular type of gynecomastia, so subcutaneous mastectomy was done. Simons classification is used for the treatment of gynecomastia, which is based on the breast size and skin redundancy. Grade 1: Minor breast enlargement without skin redundancy Grade 2A: Moderate breast enlargement with no skin redundancy Grade 2B: Moderate breast enlargement with minor skin redundancy Grade 3: Gross breast enlargement with skin redundancy that simulates a pendulous breast Groups I and II require no skin excision, but in group III the breast development is so marked that excess skin needs to be removed, and in these cases a mastopexy procedure is required [11]. These difficult cases are the only ones requiring a surgical incision out with the areola. All tissue removed should be sent for histological examination in order to exclude malignancy, as about 1% of all primary breast tumors arise in men and breast cancer accounts for 0.7% of all male cancers. Usually, mastectomies are done based on the clinical presentation of the patient. In our case, the patient benefited from a subcutaneous mastectomy using an infra areolar incision, which was proved beneficial to him physically and psychologically. | ||||||
|
Conclusion
| ||||||
|
The 46XY karyotype with enlarger satellites of acrocentric chromosome 15ps+ is one of the rare entities. Occurrence of giant gynecomastia in the presence of this particular chromosomal aberration is also a rare entity. Subcutaneous mastectomy with a cosmetically beneficial incision served the purpose of treating our patient. So every young patient presenting with gynecomastia should be evaluated for the etiology and treatment should be individualized. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Manuneethimaran Thiyagarajan – Acquisition of data, Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Pragnya Chigurupati – Substantial contributions to conception and design, Revising it critically for important intellectual content, Final approval of the version to be published Balaji Singh K. – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2014 Manuneethimaran Thiyagarajan et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|